
Those in the healthcare marketing industry can likely speak to the significant obstacles that exist when it comes to patient insights. In a previous blog post1, I outlined some of the industry-wide challenges, such as low completion rates, low respondent engagement, data quality problems and lackluster respondent experiences that contribute to even lower response rates. However, there are also intangible challenges to conducting research with patients, given that they are suffering from some disease or condition. Inherently, they are being asked to disclose a much more personal situation compared to where they shop or what brand of shampoo they use. And this sharing can evoke a lot of various emotions. Given today’s advancement of digital technology, we believe it is time to reimagine how we collect insights from patients.
I truly believe that a conversational approach offers a new solution to the unique challenges of patient research. This approach is a significant improvement on traditional mobile survey tactics. It leverages the organic interaction between individuals and their mobile devices to enhance respondent experience and unlock deeper insights — a win-win for clients and research participants alike. We believe that, within the conversational survey format, patients can respond more naturally even when discussing the sensitive topic of their disease/condition.
But, because we are researchers at heart, we don’t like to make a claim without the data to back it. We like to create a hypothesis and then test it and analyze the findings. But before we do this, we need to consider the inherent aspects to patient research.
Approaching Difficult Conversations around Health
To best understand what sets healthcare insights apart, one needs to first accept that there are inherent dynamics in conversations around healthcare that make people behave differently than they might in a study on a less personal topic. Healthcare topics can be stigmatizing, sensitive, and difficult to talk about. This is particularly true when it comes to mental health disorders; however, even in other conditions, stigmas and barriers exist. A recent study on Atopic Eczema2, for example, found a strong correlation between increased instances of depression and anxiety among those impacted by the disease. Engaging with survey participants who are experiencing emotional and physiological distress requires both enhanced empathy and a carefully curated approach to deeper understanding— and traditional quantitative survey models simply don’t cut it.
There’s also the issue of the research environment itself. While we often feel the need to leverage a qualitative setting to best capture the experiences and challenges patients face, the introduction of a moderator can trigger several emotions. And these emotions play right into the opportunity for social desirability bias in patient’s responses. Social desirability bias is, according to an NIH-funded study3, “the tendency to underreport socially undesirable attitudes and behaviors and to overreport more desirable attributes… often motivated by the desire to avoid embarrassment and repercussions from disclosing sensitive information, which is impression management.” In short, when patients are confronted with the potential judgment of a stranger who is assessing their behaviors and attitudes toward their condition, they may experience strong emotions, discomfort, or a lack of self-confidence — all of which can dramatically impact the quality and accuracy of their feedback.
Some may question whether social desirability is a real issue. After all, we can find patients willing to participate in research and, with a good moderator, many of them seem to provide candid answers. But are they? And with a self-guided survey, why would a patient not feel able to disclose?
Without the ability to compare side-by-side, we may never know. A first glimpse into this question comes from research by Meluma and Meyer4, out of The Wharton School of Business. Researchers showed that people are measurably more revealing when disclosing on their mobile device compared to their disclosure on a PC. And these findings did not even involve any personal interaction; imagine the difference that might be seen with a live interview.
Taking this one step further, an argument can also be made that the social desirability bias not only affects what gets said, but also likely influences who chooses to speak about their experience. Patients who experience heightened stigma and emotional distress are likely the ones least willing to participate in traditional qualitative research.
Responding to the Patient’s Research Experience
Knowing that sharing personal information about a condition is not typically an enjoyable experience whether in a qual or quant setting, along with the social desirability bias that likely plagues patient insights, there is need for novel approaches to patient research. We feel that Conversational Insights provides a robust solution to the inherent challenges in patient research.
To test our hypothesis that our conversational approach does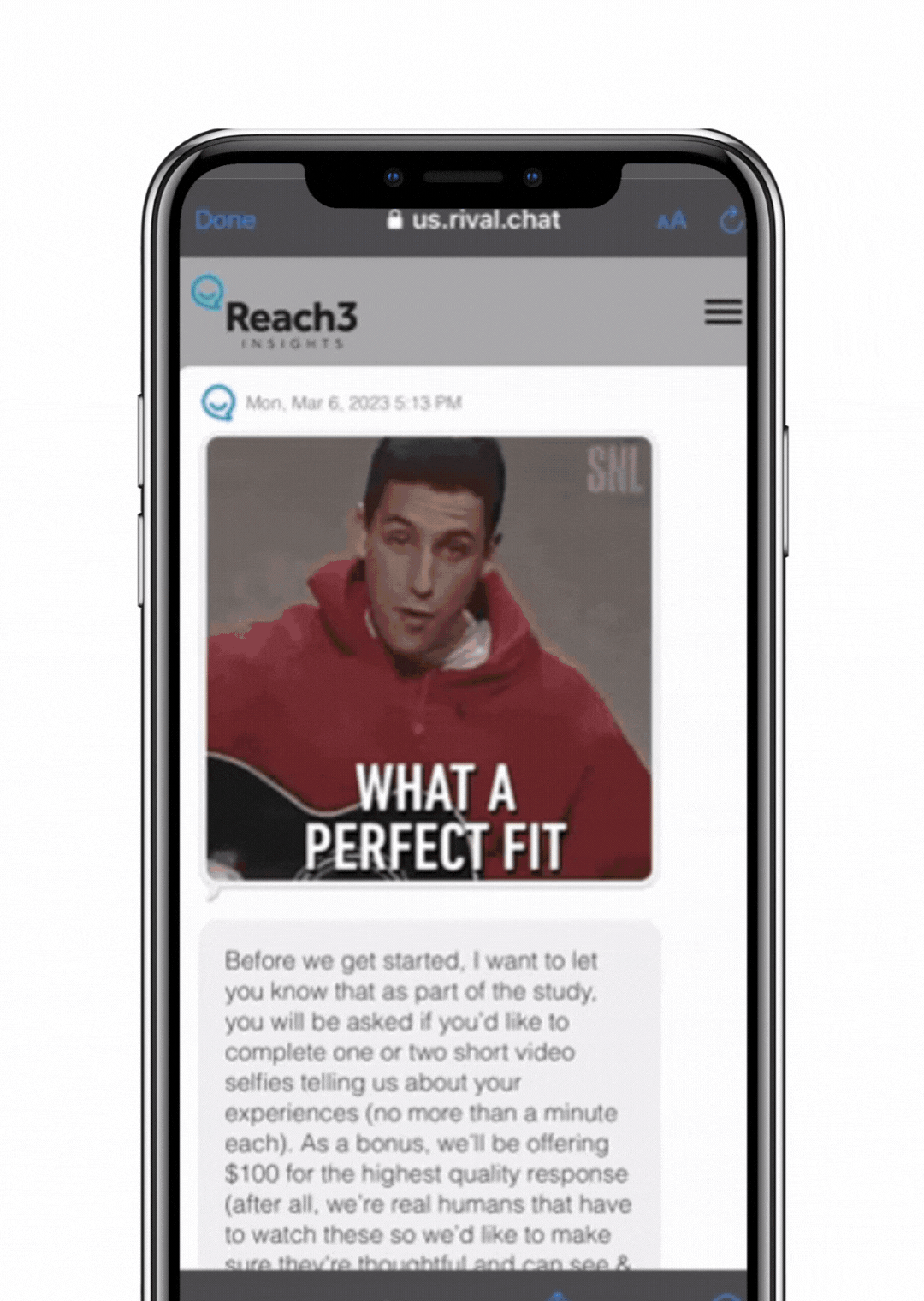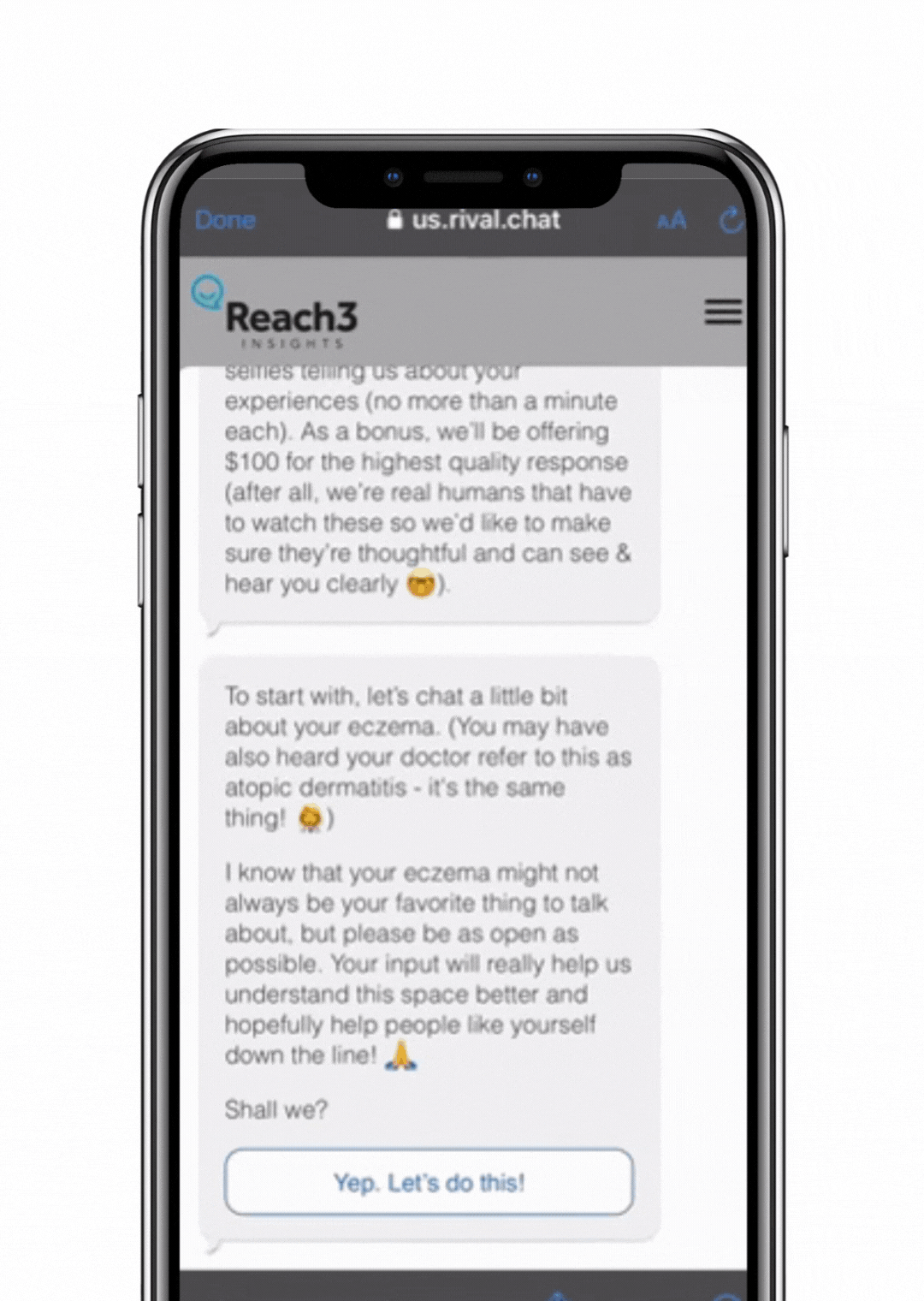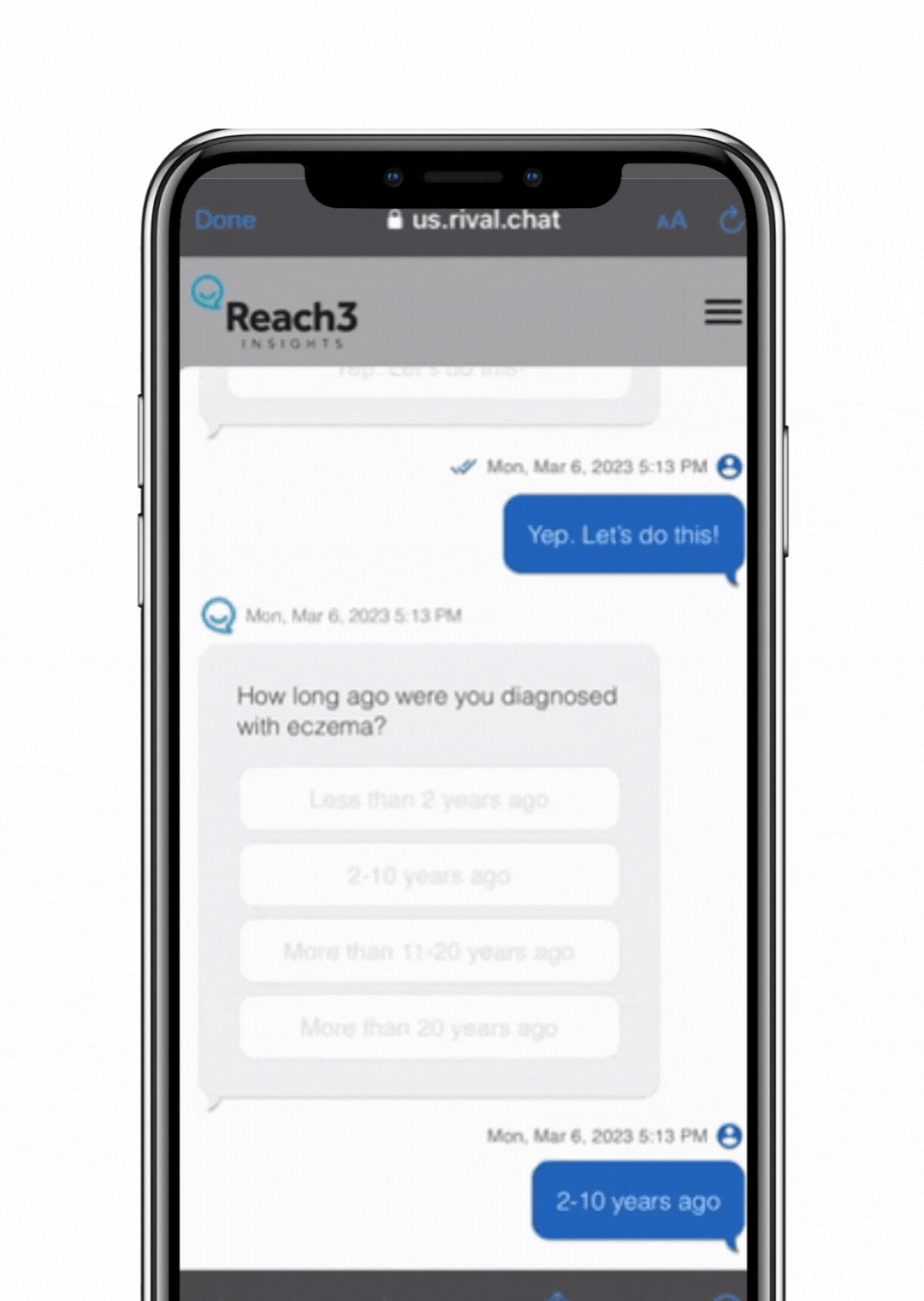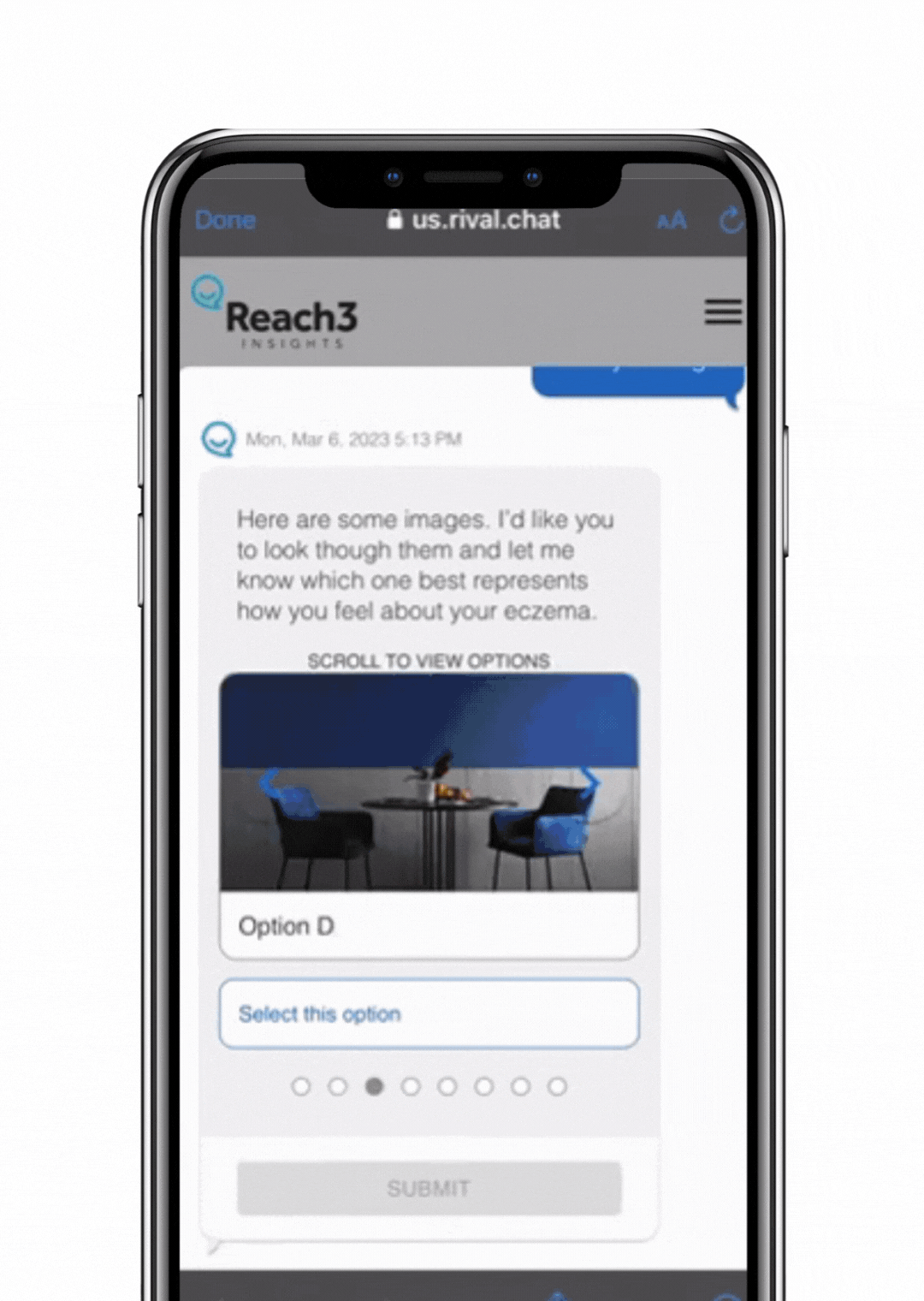 address some key challenges in patient research, we fielded a 10-minute survey to 220 eczema patients in the US, using a monadic design comparing Reach3’s conversational chat survey approach to that of a traditional ask-answer, paginated online survey. In order to measure differences in their experience and behaviors, we had individuals suffering with eczema answer a battery of questions about their disease history, thoughts and experiences related to eczema, including four open-ended questions. At the very end, we asked about their experience participating in the research.
address some key challenges in patient research, we fielded a 10-minute survey to 220 eczema patients in the US, using a monadic design comparing Reach3’s conversational chat survey approach to that of a traditional ask-answer, paginated online survey. In order to measure differences in their experience and behaviors, we had individuals suffering with eczema answer a battery of questions about their disease history, thoughts and experiences related to eczema, including four open-ended questions. At the very end, we asked about their experience participating in the research.
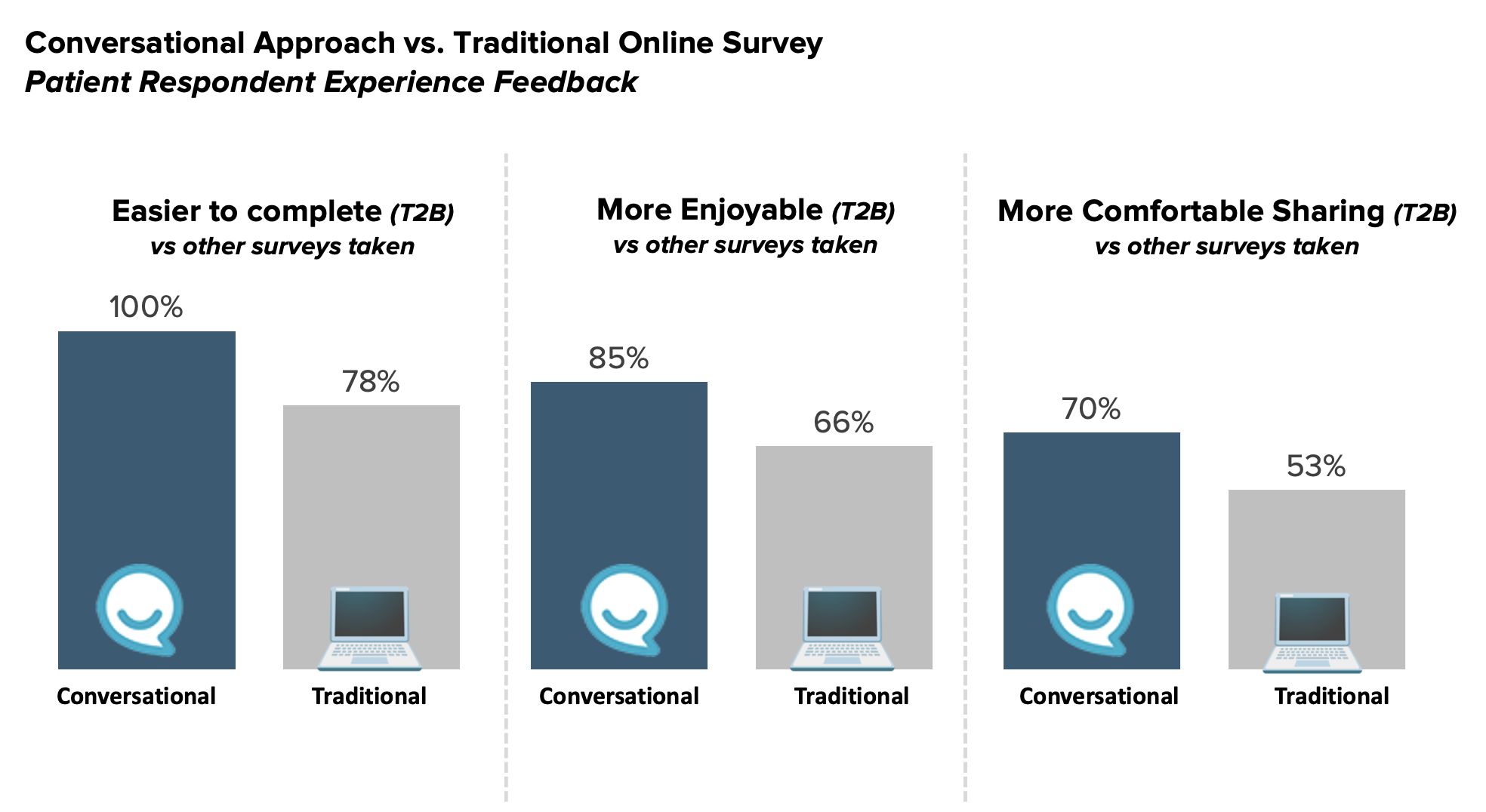
These survey experience questions, included scaled ratings on metrics, such as “easy-to- complete" and “an enjoyable experience”. One-hundred percent of patients taking the conversational chat survey agreed it was easy to complete compared to 78% for the traditional survey. And 85% said the chat survey was enjoyable compared to 66% taking the traditional format.
Our last question of the study directly inquired about their level of comfort in sharing sensitive information, followed by an open-end explanation of their rating. To our surprise, patients in the conversational group not only reported greater comfort with providing sensitive details, but at a rate nearly double that of traditional surveys: 47% vs. 25% TB (and 70% vs 53% T2B).
While the quantitative results supported our hypothesis, the qualitative open-end analysis left little doubt as to the benefits of conversational. Responses from patients via video selfies, clearly suggest Reach3 conversational chats offer the ability to add qualitative depth that can't be duplicated with traditional quantitative surveys.
- Open-end responses in the form of selfie videos via Reach3’s conversational chats, generated nine times more words than from typed responses in the corresponding traditional survey.
- Patients that typed their OE response in the conversational chat provided 2x as many words compared to the traditional survey group.
Because we know that more words doesn’t necessarily equal more revealing responses, we dug deeper. In looking at the actual open-end responses, the quotes spoke for themselves on the topic of patient disclosure and authenticity.
- I do admit I felt more open about sharing my thoughts and experiences…this survey was very enjoyable, even though I had to dive into some not so fun topics. –Prefer to self-describe, Gen Z
- I liked that this survey was considerate of how comfortable I may be answering certain questions. –Female, Millennial
- I thought the survey read very respectfully. It was both encouraging and respectful. I like that it acknowledged pronouns. I felt by the end of the survey, like I would have trusted giving information like, you know, my age or my location zip code, even down to like my sexual orientation. – Female Gen Z
A More Revealing Path in Patient Insights
In conclusion, our research-on-research shows that patients not only find a conversational approach a more comfortable environment to address an uncomfortable topic; it also enables qualitative richness and candor on a quantitative scale that would be difficult and costly to accomplish via live interviewing. Hence, we feel confident in concluding that our Conversational Insights approach and tech (chat surveys) offer an innovative solution to patient research that truly delivers deeper, more authentic insights.
So, next time you think about doing patient research that involves:
- a particularly sensitive topic;
- a topic where candor is critical but not expected;
- the need for quantitative scale but with actionable qualitative insights
or really any other critical patient research….a conversational approach may be your answer!
To learn more about Reach3s conversational approach or to contact the author, please click here.
References:
- The Time is Now to Reimagine Insights in Health. K. Palmer Sept 1 2022. Blog published Sept 1, 2022 on reach3insights.com
- Yochai Schonmann, Kathryn E. Mansfield, Joseph F. Hayes, Katrina Abuabara, Amanda Roberts, Liam Smeeth, and Sinéad M. Langan. Atopic Eczema in Adulthood and Risk of Depression and Anxiety: A Population-Based Cohort Study J Allergy Clin Immunol Pract. 2020 Jan; 8(1): 248–257
- A. Latkin, C. Edwards, M.A. Davey-Rothwelland K. E. Tobin. The relationship between social desirability bias and self-reports of health, substance use, and social network factors among urban substance users in Baltimore, Maryland. Addict Behavior. 2017 Oct; 73: 133–137
- Shiri Melumad and Robert Meyer Full Disclosure: How Smartphones Enhance Consumer Self-Disclosure. Journal of Marketing. Volume 84, Issue 3



.jpg?width=352&name=Digital%20Health%20Trends%202024%20Report%20from%20Reach3%20Insights%20(1).jpg)